
How Big Data Can Save Lives at the Hospital

As a trauma nurse at one of the largest hospitals in the country, Charles Boicey saw his share of sickness and injuries, amazing recoveries and unfortunate deaths. But for all the good he and his fellow clinicians were able to do, Boicey was frustrated that he didn’t have the information to do more. Now, as chief innovation officer at big data healthcare startup Clearsense, Boicey is determined not to let any more potentially lifesaving data slip away.
Modern electronic medical record (EMR) applications are the systems of record in most hospital settings. However, most EMRs only record patient data on an hourly basis. That’s too coarse of a sampling frequency to enable machines to detect meaningful patterns in the data. And unless busy doctors and nurses are staring at the monitoring equipment in the intensive care unit (ICU) for each patient, they’re not going to be able to catch everything.
“In that environment, which is a very fast paced environment, we missed a few things,” Boicey tells Datanami about his experience as a clinical trauma nurse at the 600-bed Los Angeles County Hospital. “We didn’t necessarily have the capabilities to catch events as they happen in a real-time nature, and that really bothered me.”
It bothered so much that he decided to go back to school and figure out how he could collect more data from patients, and how he could turn it into better insights to improve patient care. In an academic career that spanned Stony Brook Medicine and UC Irvine, he sought answers to his questions.
Big Data Search
From 2009 to 2010, he explored new big data technology being developed by the likes of LinkedIn, Twitter, Facebook, Yahoo, and Google. “Those technologies really opened up some possibilities in healthcare, taking us out of relational world into an infrastructure that would support some of the things we weren’t able to do,” he says. “I learned a lot during that year.”
Boicey started exploring different technologies, stating first with MongoDB‘s NoSQL database and later with Hadoop. With both MongoDB and Hadoop, Boicey exceeded what he could do with relational technology.
“We had to make choices of what goes into those [analytic] environments,” says Boicey, who holds MS and RN-BC degrees. “I couldn’t load everything that came from the laboratory system, pathology or other ancillary systems, or the data from the instruments.”
Boicey eventually settled on Hadoop as the basis for his work — a healthcare analysis system he started developing at UC Irvine that could ingest large sums of clinical and operational data and make useful predictions on patient outcomes. Only Hadoop, he says, allowed him to ingest massive amounts of data.
“Anything that put off a signal, we took it and landed it in HDFS,” he says.
Hadoop Landing
Eventually, Boicey left academia and joined Clearsense, a Jacksonville, Florida-based company that was spun out of the healthcare IT specialist firm Optimum Healthcare IT. There, he helped harden the Hadoop-based analytics system for three use cases, including analyzing clinical, operational, and financial data.
Hadoop is the best repository for this data because it allows Clearsense to land the data first, and make sense of it later. “That’s really important because in healthcare, we’re not quite there as far as our maturity model in handling data and analytics,” he says. “I have no idea what the future use cases would be for this data, but at least I have them.”
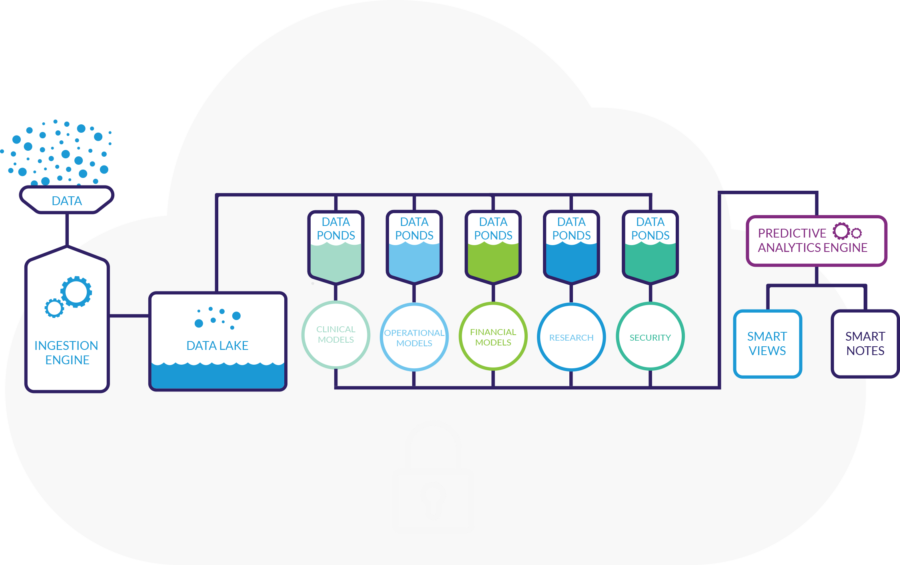
The Clearsense Inception architecture
Like most big data projects, transforming the raw data into useful information is the goal of Clearsense’s system, which is called Inception. The software utilizes a variety of tools in Hortonworks Hadoop stack, including HDFS, MapReduce, YARN, HBase, Sqoop, Spark, NiFi, Atlas, and Ranger.
Better Monitoring
“I started bringing in physiological monitoring data at one minute intervals, so everything off the monitoring systems, as well as everything off of ventilators, smart pumps, etc,” Boicey says. “We’re monitoring every minute as opposed to bringing vital signs every hour, so we’re able to spot the trends much earlier than had been in the past.”
Clearsense monitors upwards of 40 separate data feeds for patients in the intensive care unit (ICU), or perhaps eight feeds for a patient in a regular bed. All that data is critical to Clearsense’s machine learning work, which is primarily programmed in R and executed in Spark.
All that data provides a testbed upon which to train the classification algorithms to identify what a “normal” state looks like. During inference, the algorithms continually analyze the stream of data to detect any anomalies that could indicate a deterioration of the patients’ condition.
Real World Impact
Boicey says Inception, which has been deployed in six production clients, has proven capable of giving nurses and doctors a 30 minute to two hour cushion that something is about to happen with a patient.

Charles Boicey, chief innovation officer, Clearsense
“Clinically the reliance is on us for keeping very busy clinicians aware of what’s going on at any particular time,” he says. “It gives the clinicians the information, such as the heartrate has increases by X, the blood pressure has decreased, urine output has decreased, something is going on here.”
The data formed the basis for a variety of models, including sepsis detection and patient deterioration models. All in all, the models contribute to better situational awareness.
“Because we’re getting the physiological monitoring data as well as the laboratory data and other data in a real-time nature, we’re able to present clinicians with a really good clinical picture of a patient at any given time,” Boicey says. “We’re not telling you what to do. We’re just showing you that your patietnt’s conditions is changing and allow you to do something with that.”
Inception is still fairly new, as it’s been live for just a matter of months at client sites. Eventually, Clearsense hopes to push the ball forward in the healthcare analytics space. “Our hope is that we’ve made enough of an impact that we’ve make it easier for them to adopt these technologies,” Boicey says.
However, the entire space is moving slowly. Unless you happen to find yourself in one of the country’s cutting-edge hospitals, like Geisinger Health, Mercy Health, or the Cleveland Clinic — all of which have created their own systems – you won’t likely to find your vitals being monitored in real time by machine learning algorithms.
“We’re a ways off,” Boicey says. “But my goal has always been to offer the same analytical capability that a 50-hosptial network enjoys to a 50-to-75 bed hospital.”
Related Items:
Using Big Data to Its Full Potential in Healthcare
3 Key Steps to Transforming Healthcare with Predictive Analytics






























